MissionVet Specialty & Emergency


Emergency Services
Available 24 hours a day including weekends and holidays for pets in need. Check-in online and wait from the comfort of your home.
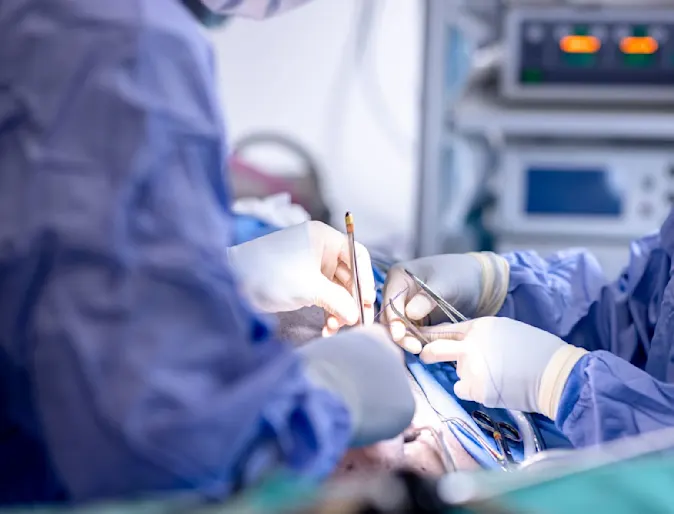
Specialty Services
Advanced medical care for your pets, in collaboration with your family veterinarian. Our team is composed of industry leaders, pioneers, and board-certified experts.

Veterinarian Portal
We strive to maintain strong relationships with our veterinary partners. Our veterinarian portal helps to enhance communication, collaboration, and patient care.
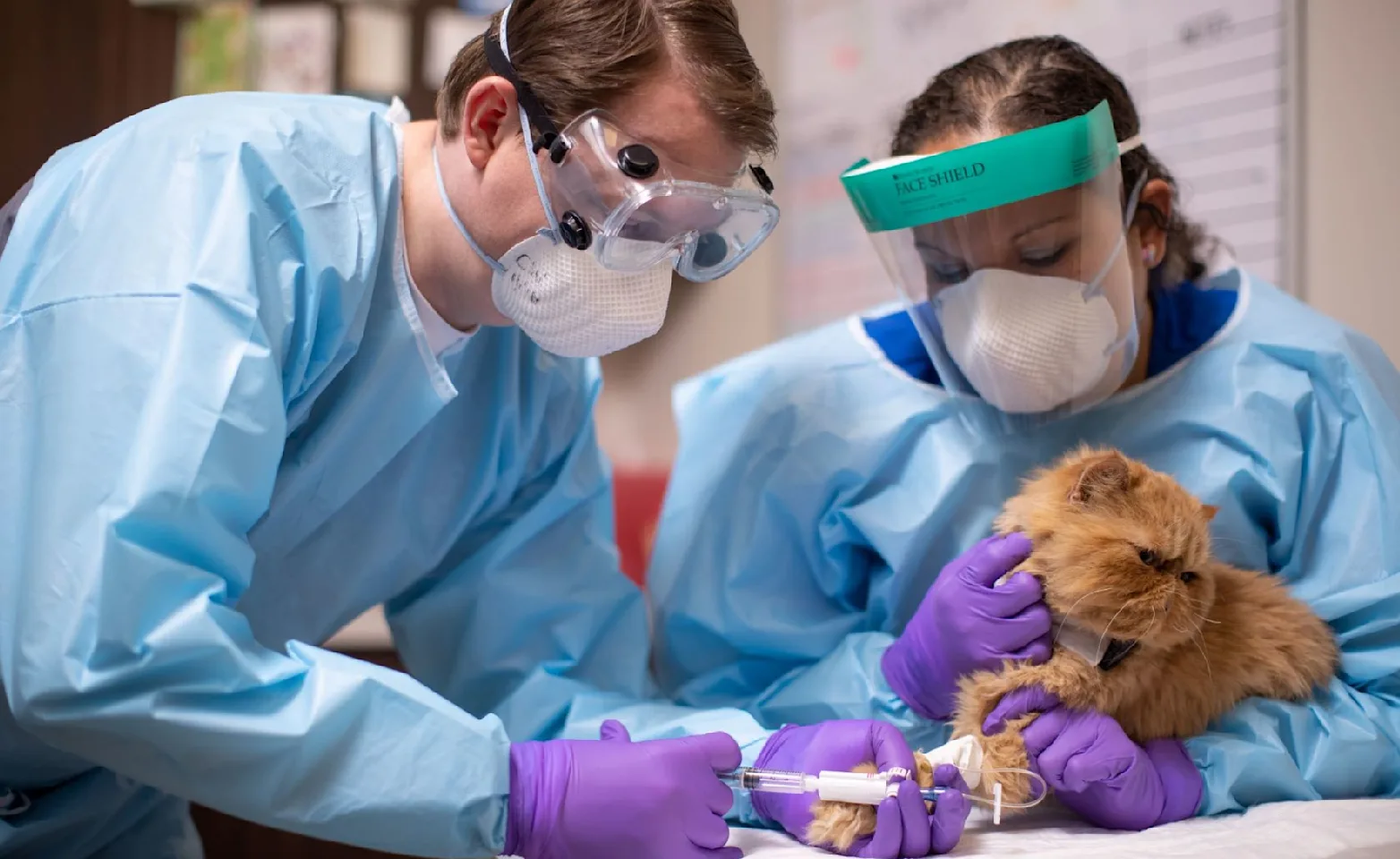
Pushing the limits of what is possible
We believe passionately in pushing the boundaries of what is possible in veterinary medicine. Our team is composed of industry leaders, pioneers, and board-certified experts. With our focused efforts, we are actively accelerating the veterinary field to a brighter future - one with revolutionary techniques and uncompromising standards.
Client Testimonials & Reviews
We at MissionVet Specialty & Emergency have been dedicated to providing quality veterinary care to the San Antonio, TX community since 2012. Here’s what some of your neighbors are saying about us.

